Is Mouth-Breathing Really the Villain Everyone’s Talking About?

“Your child asleep, mouth open, snoring softly, sounds familiar?- Looks harmless, right? Maybe even cute?”
What if I tell you that this simple habit is quietly reshaping their face, affecting sleep, and even behaviour?
Mouth-breathing isn’t just a quirk; it’s a signal that your child’s airway may not be healthy.
Here’s why mouth-breathing deserves more attention than it gets and what parents can do about it.
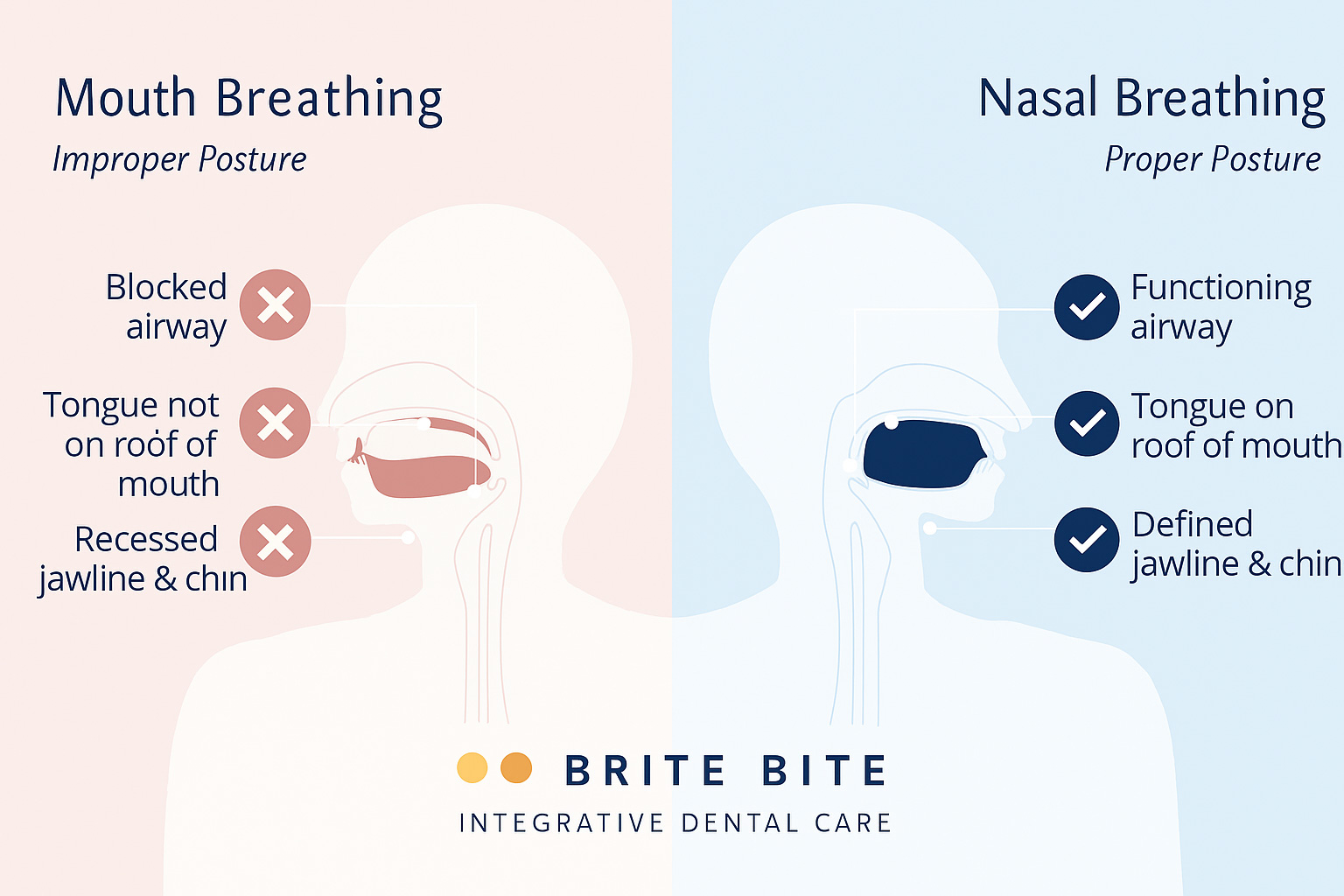
Nasal Breathing vs Mouth Breathing
Why Nose Breathing Is Essential for Your Child’s Health and Development
Breathing through the nose does more than just move air in and out. It filters, humidifies, and warms every breath before it reaches the lungs keeping the airways protected from dust, allergens, and bacteria.
When your child breathes through the nose, their tongue naturally rests against the roof of the mouth (the palate).
This gentle upward pressure helps the jaws grow wide and balanced, while the mouth stays moist and healthy.

What Really Happens When Your Child Breathes Through Their Mouth instead of Their Nose?
When a child breathes through their mouth instead of their nose, the body’s natural defenses take a hit. Mouth breathing skips the nose’s natural filters, letting dry, unfiltered air reach the throat and lungs.
This dries out the mouth and throat and to protect itself the body produces extra mucus or phlegm which is why many children wake up congested, even if they weren’t sick.
Without nasal filtration, germs and allergens enter more easily, increasing the risk of colds, sore throats, and allergies. Over time, this repeated exposure can inflame the tonsils and adenoids, making nasal breathing even harder and deepening the mouth-breathing cycle.
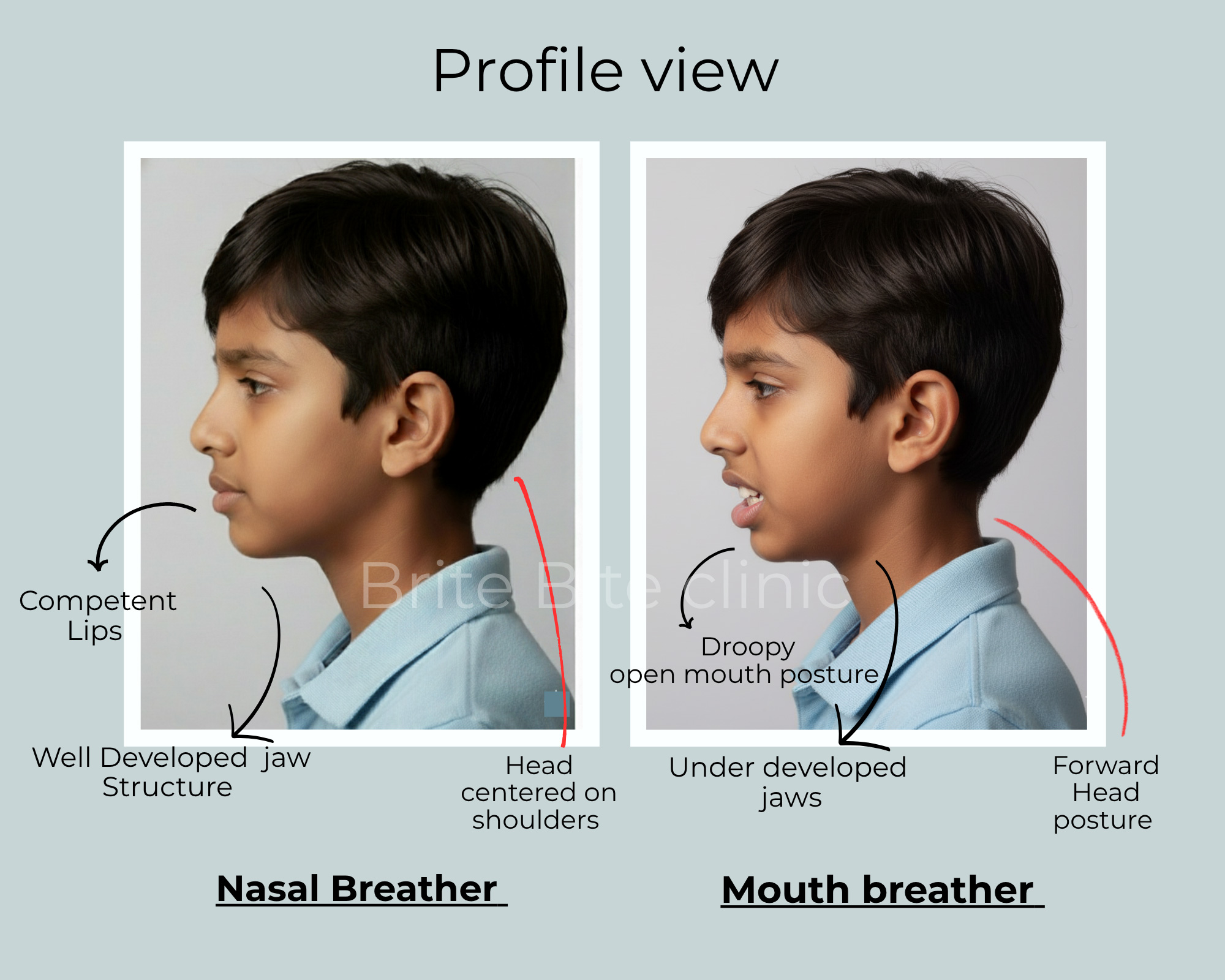
How Mouth Breathing Affects Your Child’s Teeth, Jaw, and Facial Growth
When the mouth stays open, the tongue drops down instead of resting against the palate. Without that gentle upward pressure, the upper jaw loses its natural guidance for growth and can become narrow over time. This often leads to crowded or misaligned teeth, unclear speech sounds (especially sounds like “s,” “sh,” “ch,” and “t”), and an improper swallowing pattern all of which further affect how both the upper and lower jaws develop.
A dry mouth also means less saliva to wash away bacteria, making cavities more likely and often causing bad breath.
What starts as a simple breathing habit can gradually influence how your child’s face grows, how clearly they speak, and how healthy their teeth stay.

How Mouth Breathing Disrupts Sleep and Affects Behaviour in Children
Over time, mouth-breathing can disturb deep sleep and even be an early warning sign of sleep-disordered breathing or childhood sleep apnea.
When the brain doesn’t get enough oxygen through the night, children may appear hyperactive,fidgety, have difficulty with emotional regulation or have trouble focusing during the day.
Sometimes, what looks like “restlessness” or “poor attention” is actually a breathing problem in disguise.
When Mouth-Breathing in Children Becomes a Concern
Occasional mouth-breathing during a cold or allergy is completely normal, but if your child breathes through their mouth most of the day or night, even when they’re not sick or congested, it may be a sign of something deeper.

What Causes Chronic Mouth Breathing in Children?
- Enlarged tonsils or adenoids
- Chronic nasal blockage
- Habitual Open-Mouth Posture
- Tongue Tie or Low Tongue Posture
- Narrow Airway or Sleep-Disordered Breathing
- Low Oral Muscle Tone
- Facial or Dental Structure Issues
How Parents Can Help Correct Mouth Breathing Early
The good news? Mouth-breathing can often be corrected especially when caught early. Spend a few days observing your child while they’re awake and asleep. If you notice an open mouth, snoring, or tired mornings, consult a pediatric or airway-focused dentist. Book your child’s screening.
Ready to Book a Consultation?
Let our team at The Brite Bite Clinic assess your child’s breathing, airway, and facial growth early before it impacts their long-term development.
Our Approach to Mouth Breathing at The Brite Bite Clinic
At The Brite Bite Clinic, we don’t just treat teeth, we look at how your child breathes, sleeps, and grows. Correction isn’t cosmetic; it’s developmental.
Our integrative approach includes airway screening, growth assessment, ENT collaboration, and myofunctional therapy, supported by orthodontic monitoring when needed. We also assess tongue posture and oral habits that can impact healthy breathing and jaw growth. Learn more about our airway assessments.
FAQs
- Do kids outgrow mouth breathing?
- If the child has developed mouth breathing due to short-term colds or allergies then yes the child should not develop a daily habit. But if you see your child habitually breathing from the mouth even in the absence of a cold or an allergy it often won’t go away on its own and needs intervention.
- How do I stop my child from mouth breathing?
- Start by observing their breathing habits while awake and asleep. Then consult an airway-focused pediatric dentist to identify the root cause and explore treatment options like habit correction, myofunctional therapy, or airway support.
- What age can you fix mouth breathing?
- Ideally, as early as age 3–5 when growth patterns are still adaptable. However, meaningful changes can still be made in older children and even teens.
- What is an adenoid face?
- An “adenoid face” refers to facial changes seen in some children with chronically enlarged adenoids. When adenoids block the nasal airway, kids often breathe through their mouth which can lead to a long, narrow face, open lips, a high-arched palate, and even dental crowding.This facial pattern can develop slowly over time if mouth-breathing isn’t corrected early.
- Can an adenoid face be reversed in children?
- Yes if caught early. When breathing patterns and tongue posture are corrected before facial growth is complete, changes to jaw development and posture can often be improved or reversed.
- Is mouth breathing normal in children?
- Occasionally, yes, like during a cold. But chronic mouth breathing is linked to dental issues, sleep problems, poor posture, and altered facial growth. It’s not ideal as a long-term breathing pattern.
- Can mouth breathing cause behavioral issues?
- Yes. It can reduce oxygen and disrupt sleep, which may lead to poor focus, irritability, hyperactivity, or even ADHD-like symptoms.
- Is mouth breathing linked to ADHD or Autism?
- Mouth breathing can mimic ADHD-like behaviors (like hyperactivity or poor attention), but it’s not a direct cause of ADHD or Autism. However, both ADHD and Autism can co-occur with breathing and sleep issues, so an airway evaluation is often helpful.
- Can mouth breathing cause sleep apnea in children?
- Yes, it can. Chronic mouth breathing is often linked to sleep-disordered breathing, including pediatric obstructive sleep apnea. It may be caused or worsened by enlarged tonsils, a narrow airway, or poor tongue posture. If your child snores, sleeps restlessly, or wakes up tired, it’s worth getting their airway evaluated.
References
1. American Academy of Pediatric Dentistry. (2023). Guideline on Management of the Developing Dentition and Occlusion in Pediatric Dentistry.
https://www.aapd.org
2. Guilleminault, C., Huseni, S., & Lo, L. (2016). A frequent phenotype for paediatric sleep apnoea: short lingual frenulum. European Respiratory Journal, 47(6), 168–177.
3. Villa, M. P., et al. (2015). Sleep-disordered breathing and behavioural problems in children. Sleep Medicine Reviews, 20, 29–35.
https://doi.org/10.1016/j.smrv.2014.06.007
4. Huynh, N. T., Morton, P. D., Rompré, P. H., & Papadakis, A. (2011). Associations between sleep-disordered breathing and facial growth in children. Sleep Medicine Reviews, 15(6), 463–475.
5. American Academy of Sleep Medicine. (2022). Pediatric Obstructive Sleep Apnea (OSA): Clinical Guidelines and
Diagnosis Criteria.
https://www.sleepfoundation.org
6. Graber, L. W., & Vanarsdall, R. L. (2011). Orthodontics: Current Principles and Techniques (5th ed.). Elsevier.
7. Harari, D., Redlich, M., Miri, S., Hamud, T., & Gross, M. (2010). The effect of mouth breathing versus nasal breathing on dentofacial and craniofacial development in orthodontic patients. Laryngoscope, 120(10), 2089–2093.
8. Abreu, R. R., Rocha, R. L., Lamounier, J. A., & Guerra, Â. F. (2008). Etiology, clinical manifestations and concurrent findings in mouth-breathing children. Journal de Pediatria, 84(6), 529–535.



